Uganda
In Uganda, more than 95 percent of the country has stable malaria transmission, with malaria infections occurring all year round. Although malaria affects both men and women of all ages, gender and youth dynamics play a key role in determining health outcomes for individuals. Maternal, newborn and child health indicators are poor, unevenly distributed across the country and worse in specific vulnerable populations – 28 percent of maternal deaths occur in young women aged 15 to 24 years – and there here remains a shortage in healthcare workers. We work with the Ministry of Health and project partners to improve integrated community case management and strengthen disease surveillance, identifying gaps in coverage through the lens of gender and youth.
iCCM+ : Access to quality health services for childhood diseases and MNC in 14 districts of Uganda
Through this follow-up to the 2015–2018 Integrated Community Case Management – Maternal and Child Survival (iCCM-MaCS) project, we worked with the Ministry of Health to strengthen referral systems for under-fives with danger signs, and deliver integrated community level services for maternal, newborn and child health, nutrition, and water, sanitation and hygiene in three districts in the Tooro region: Bunyangabo, Kabarole and Kamwenge.
Strengthening Uganda's response to malaria
The Strengthening Uganda’s Response to Malaria (SURMa) project builds community-level capacity to diagnose and treat malaria, taking the fight against malaria to the household level, highlighting the roles individuals can play in preventing transmission. To promote ownership and ensure sustainability, project activities are delivered by the respective districts, with Malaria Consortium providing technical support and supervising village health teams (VHTs) and community health extension workers (CHEWs).
Regional health integration to enhance services in eastern Uganda
Within the broader scope of the Regional Health Integration to Enhance Services in Eastern Uganda (RHITES-E) project, Malaria Consortium is supporting 25 districts in eastern Uganda with the delivery of malaria prevention and treatment interventions, as well as with maternal, newborn and child care activities.
Optimising a digitised community health toolkit in Buikwe, Uganda: Improving equitable healthcare access through digital technologies
Malaria Consortium and partners are providing technical assistance to the Ugandan government to update and introduce the integrated community case management module of a digitised community health toolkit, which aims to digitise all areas of community health, advance universal health coverage and achieve health equity.
Determining the malaria burden and long-term complications following SARS-CoV-2 infection
This study is taking place in Ethiopia and Uganda. It uses both qualitative and quantitative approaches and a case-control study design to explore the relationship between past SARS-CoV-2 infection and malaria risk.
Supporting Uganda’s Malaria Reduction and Elimination Strategy (SUMRES)
Malaria Consortium is establishing a functional integrated community case management (iCCM) programme in the northern Uganda Lango and Acholi regions through the Supporting Uganda’s Malaria Reduction and Elimination Strategy (SUMRES) project. It aims to reduce morbidity and mortality due to malaria and other common illnesses
Malaria control in Ebola-affected districts in Uganda
Through the UNICEF funded project, Malaria Consortium will be supporting the project to strengthen the Ebola Virus (Sudan strain) outbreak in Mubende and Kasanda. The outbreak response includes Malaria Mass Drug Administration (MDA), LLINs Distribution & Malaria Risk Communication as priority actions.
Malaria Consortium in Uganda
In Uganda, we have led in the distribution of long-lasting insecticidal nets (LLINs)– through mass distribution campaigns as well as continuous distribution at health facilities. Through our work on integrated community case management (iCCM) and social and behaviour change (SBC), we provide evidence to scale up innovative approaches to target malaria and other childhood diseases. Our implementation research supports the strengthening of surveillance systems and monitoring and evaluation efforts to ensure the timely use of quality data.
In support of Uganda’s National Malaria Control Strategy, USAID’s five-year Malaria Action Program for Districts (MAPD), which ran from 2016-2021, Malaria Consortium sought to reduce maternal and childhood morbidity and mortality due to malaria.
Together with Banyan Global, we conducted a qualitative study to identify how gender- and youth-related norms might be hindering effective malaria control in Uganda.
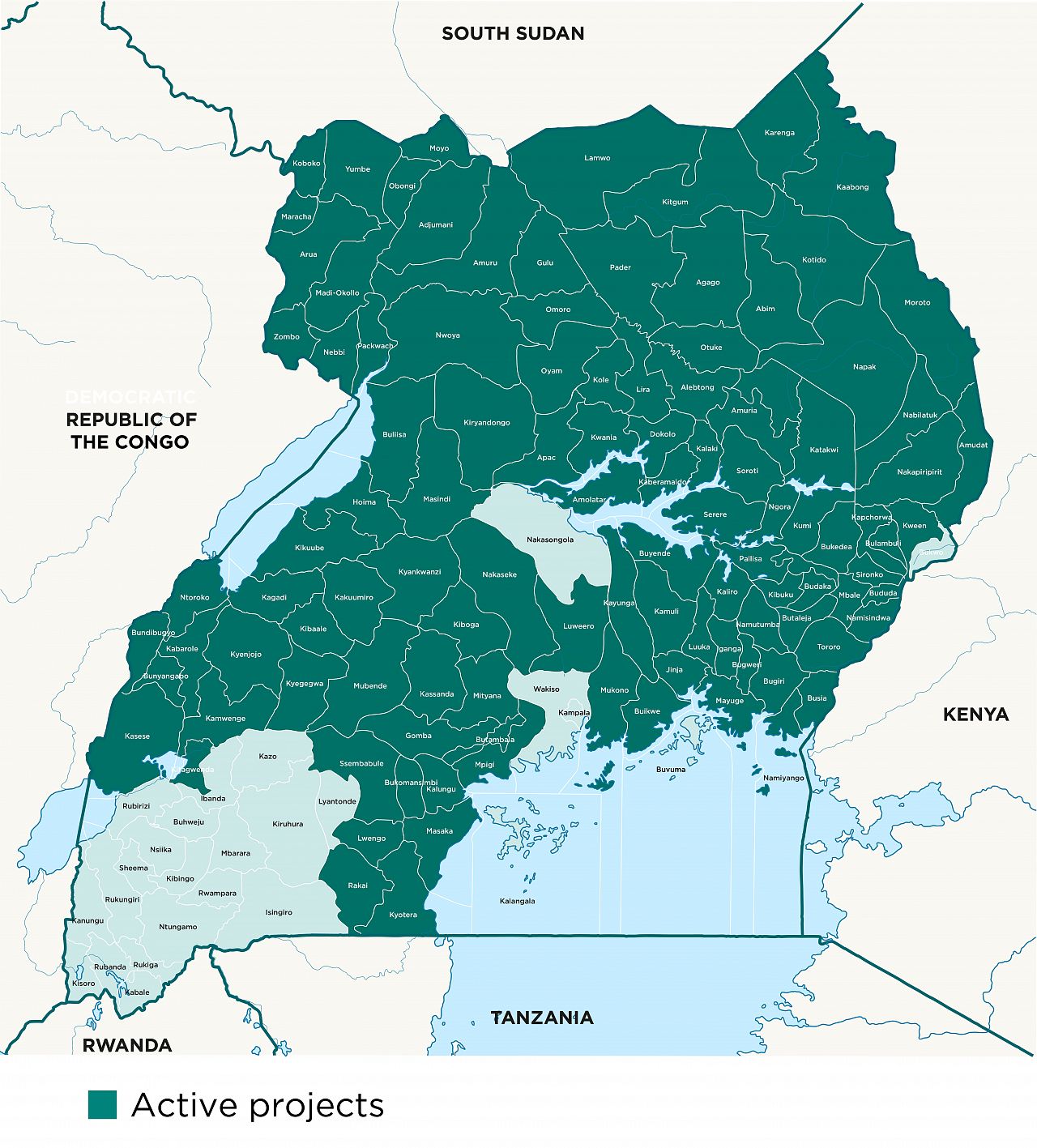
Areas of focus
Together with Banyan Global, as part of USAID’s Malaria Action Program for Districts (MAPD), we identified barriers related to gender and youth that hinder effective malaria control and prevention. We trained district health management teams, health workers and community leaders. We engaged communities, providing young people with the necessary skills, knowledge and resources to drive discussions on malaria prevention and control. Consequently, we worked with them to identify solutions to address the negative effects of inequitable gender and youth practices on their decision-making.
We implement innovative communication interventions to facilitate sustainable behaviour change. In 2018, we launched the Giving malaria the boot! campaign, using FIFA World Cup matches to increase men’s knowledge around malaria prevention. Before matches, football commentators spread social behaviour change (SBC) messaging, reaching over 7.5 million people via radio spots and over 197,000 people through mobile cinemas and community dialogues.
This messaging emphasised the importance of consistent use of long lasting insecticidal nets (LLINs), seeking early treatment and adhering to prescribed medication — leading to an increase in expectant mothers’ use of LLINs and uptake of intermittent preventive treatment in pregnancy (IPTp).
To strengthen Uganda's health system, we provide technical assistance to governments and programmes to deliver the best possible services and maximise available resources. To increase access to healthcare services in remote areas of Uganda, we helped the MoH improve iCCM of common childhood illnesses by providing technical support and supervision to village health teams (VHTs) and community health workers (CHWs).
Since 2015, we have supervised, trained and equipped more than 40,000 VHTs to diagnose and treat pneumonia, malaria and diarrhoea in children under five, training VHTs to refer children with warning signs and symptoms to nearby health facilities for further investigation and treatment.
Together with the National Malaria Control Division (NMCD), we started a phased implementation study in three districts in the Karamoja region in 2021 to evaluate the acceptability, feasibility and impact of seasonal malaria chemoprevention (SMC). While its efficacy has been proved in regions in the Sahel with low resistance to the antimalarials administered, it has not been evaluated in areas with high resistance. We will also document the coverage and quality of implementation and our results will inform a potential scale-up of SMC in other high-resistance areas in Uganda.
In Uganda, we support government and health facility staff to improve data quality and use. We are developing the capacity of health facility staff to actively monitor malaria trends through routine data gathering, enabling them to predict malaria upsurges and pinpoint hotspots for targeted interventions.
We have created sub-county geospatial maps, which combine temporal and spatial information with traditional data to build data visualisations. These allow the Ministry of Health to identify areas with high malaria incidence and test-positivity rates, and to design appropriate responses.
In Uganda, we responded to the COVID-19 pandemic by developing the capacity of more than 30,000 frontline health workers to identify, treat and refer cases of COVID-19. We also guaranteed access to essential personal protective equipment.
To help the Ministry of Health slow the spread of the virus, we disseminated information and education materials — such as posters and pamphlets — via house visits, radio broadcasts, social media and SMS to inform and sensitise communities about COVID-19 and appropriate health-seeking behaviours.
Related content
 Page:
Page:Webinar: Catalysing change: The crucial role of philanthropy in eliminating malaria
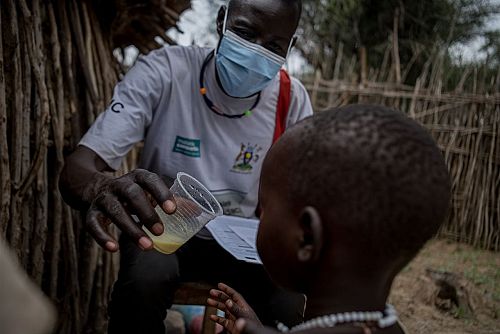 Page:
Page:Seasonal malaria chemoprevention
 Resource: Presentation
Resource: PresentationPublished 26 April 2024
A cluster randomised controlled trial to compare sulfadoxine-pyrimethamine and amodiaquine with dihydroartemisinin-piperaquine for seasonal malaria chemoprevention in Karamoja region, Uganda
 Resource: Presentation
Resource: PresentationPublished 26 April 2024
Harnessing the power of routine data for decision-making and programme improvement: Lessons from delivering seasonal malaria chemoprevention
 Resource: Presentation
Resource: PresentationPublished 26 April 2024
Cluster randomised controlled trial and quasi-experimental studies to assess the impact of seasonal malaria chemoprevention using sulfadoxine-pyrimethamine and amodiaquine in Karamoja region, Uganda
 Resource: Project report
Resource: Project reportPublished 25 April 2024
Malaria Consortium’s seasonal malaria chemoprevention programme: Philanthropy report 2023
 Resource: Project report
Resource: Project reportPublished 25 April 2024
Coverage and quality of seasonal malaria chemoprevention supported by Malaria Consortium in 2023
 Resource: Presentation
Resource: PresentationPublished 25 April 2024
Evaluating the impact of seasonal malaria chemoprevention on markers associated with drug resistance in Karamoja region, Uganda
 Resource: Presentation
Resource: PresentationPublished 25 April 2024
Evaluation of seasonal malaria chemoprevention implementation in predominantly nomadic pastoralist communities in Karamoja region, Uganda
 Resource: Poster
Resource: PosterPublished 24 April 2024
Impact of mass drug administration of dihydroartemisinin piperaquine during the Ebola virus disease outbreak on malaria morbidity and mortality in Uganda
 News:
News:Published 23 April 2024
Malaria Consortium honoured by Ugandan government for contribution to combat malaria
 Resource: Poster
Resource: PosterPublished 23 April 2024
Adverse events and reporting mechanisms for seasonal malaria chemoprevention: Insights from a survey in Karamoja region, Uganda
 Resource: Project brief
Resource: Project briefPublished 23 April 2024
Seasonal malaria chemoprevention
 Resource: Poster
Resource: PosterPublished 22 April 2024
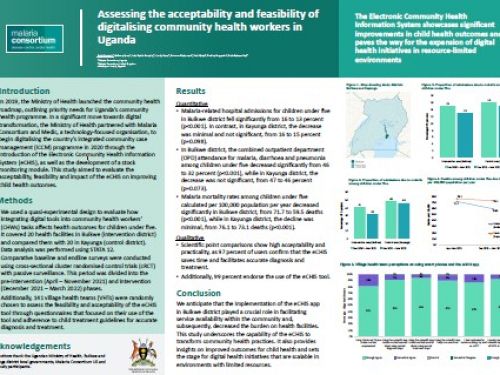
Assessing the acceptability and feasibility of digitalising community health workers in Uganda
 Resource: Poster
Resource: PosterPublished 22 April 2024
A cross-sectional survey to assess the feasibility and acceptability of seasonal malaria chemoprevention in Karamoja region, Uganda
 Resource: Project brief
Resource: Project briefPublished 28 March 2024
Strengthening Uganda’s preparedness against arboviral threats
 Page:
Page:About us
 Blog:
Blog:Published 7 March 2024
International Women's Day 2024: Seven ways to make health programmes gender intentional
 Page:
Page:International Women's Day 2024: Seven ways to make health programmes gender intentional
 Page:
Page:Our third year as an Independent Research Organisation: Using research to respond to health inequities and emerging threats
 Blog:
Blog:Published 20 February 2024
Our third year as an Independent Research Organisation: Using research to respond to health inequities and emerging threats
 Page:
Page:International Day of Women and Girls in Science 2024
 Resource: Annual review
Resource: Annual reviewPublished 2 January 2024
Trustee's report and financial statements for the year to 31 March 2023 Project:
Published 1 January 2024
Forecasting outbreak risks from extreme climate with active surveillance technology (FORECAST) Project:
Published 1 January 2024
Strengthening Uganda's preparedness against arboviral threats (SUPAAT)
 Page:
Page:The impact of Global Fund investment in fighting malaria
 Page:
Page:Top reads of 2023
 Blog:
Blog:Published 15 December 2023
Top reads of 2023