At the international border checkpoints between Cambodia and Laos, Stung Treng Province, a green booth with various messages invit......read more
Malaria Consortium’s Edward Idenu receives best practice award
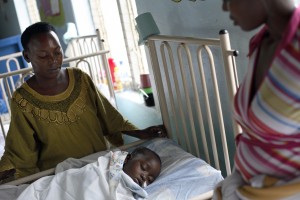
A child with severe malaria. Photo by William Daniels.
In March, Malaria Consortium was invited to a meeting in Kampala, whic......read more
Preventing malaria through drama and performance
“Our main purpose is to educate communities about malaria - its effects, how it is transmitted and how to avoid it.” Mugoya Mu......read more
Supportive supervision: improving the quality of community health services
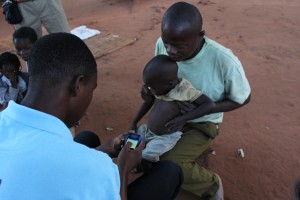
Community health workers, when trained and equipped to manage simple cases of pneumonia, diarrhoea and malaria in children under t......read more
European Year for Development launches amidst growing public support for aid
2015 is set to be an important – and hopefully transformational – year for international development. Over the next 12 months ......read more
Helping to fight malaria with positive deviance volunteers
Wanweena Tangsathianraphap, External Communications Officer for the Asia region, visited Ratchaburi province in Thailand to report......read more
Malaria Consortium’s behaviour change communication project
Monica Posada is Malaria Consortium’s behaviour change communication (BCC) technical specialist for the Asia region. She recentl......read more
Preventing the number one infectious cause of death in children
November 12th is World Pneumonia Day. To mark this occasion, Malaria Consortium interviewed Dr Phanuel Habimana, adviser on child ......read more
Helping to eliminate the threat of dengue in Cambodia with Malaria Consortium
Vanney Keo is a Malaria Consortium field assistant, who has been working in Cambodia.
I have been working for Malaria Consortium ......read more
Malaria Consortium’s RAcE project: Implementing iCCM in Nigeria
Dr Jonathan Jiya is the programme manager of Malaria Consortium’s RAcE project in Nigeria. He recently met with senior leaders o......read more