Pioneer Project - in pictures
25 February 2015
Malaria Consortium’s Pioneer project was a five-year initiative in Uganda that reduced the malaria burden in the country using a variety of effective methods. Take a look at the gallery below to learn more about the approaches to malaria control and hear from some of the people whose lives were affected by the project.
At the start of the Pioneer Project in 2009, only 19 percent of households owned an insecticide net, about a third of households lived within 10km of a health facility, and approximately 23 percent of under-five deaths in the region were due to malaria. This was a result of the moderate-to-high transmission rate, key health system challenges and limited knowledge of disease prevention practices. Pioneer sought to address these challenges by using a variety of effective methods in partnership with the Ministry of Health.
Copyright Malaria Consortium/William Daniels
One of Pioneer’s main approaches to controlling malaria was through the distribution of long lasting insecticide treated nets (LLINs). Over the course of the project, over 600,000 LLINs were distributed to 234,591 households – covering over one million people to achieve universal coverage in four districts.
Copyright Malaria Consortium
Rachel and her family use LLINs every day. “We have to protect ourselves from mosquitoes no matter whether it is a season in which people think there are fewer mosquitoes. They can attack you anytime; you are not aware.” Rachel’s attention to her family’s safety is a result of her participation in community dialogues in her village where she has learnt how to live a healthier life to prevent illnesses.
Copyright Malaria Consortium
Entomological surveillance – involving regular surveys evaluating the impact of interventions on vector density and behaviour as well as malaria transmission intensity – was one of the crucial components of the Pioneer project. “We are looking at the general behaviour of mosquitoes and more especially their feeding habits,” explains Charles Ntege, Vector Control Officer responsible for entomological surveillance in Kyankwanzi. The survey findings have shown an overall reduction in the population density of mosquitoes, entomological inoculation and human biting rates.
Copyright Malaria Consortium
Case management of malaria forms another essential pillar of malaria control. The Pioneer project ensured that cases were diagnosed properly by supporting the introduction of malaria rapid diagnostic tests (mRDTs) in 88 health facilities and trained health workers on their correct usage. The practice of testing before treating was initially met with resistance, but the benefits soon became apparent. “You don’t waste time giving treatment that is not right for the patient and delaying the treatment he really needs,” says Paul Mulindwa, a senior nursing assistant.
Copyright Malaria Consortium/Tadej Znidarcic
The introduction of RDTs has resulted in improved supply chain management and the rational use of antimalarial drugs. It also brought down drug stock outs to zero in all health facilities. The number of people who accessed free, quality, confirmatory diagnostic tests for malaria through these health centres reached 1,668,547.
Copyright Malaria Consortium
When malaria symptoms arise, young children in particular are in grave danger and may not survive without appropriate treatment. Often the distance and the cost of travel between rural households and the nearest health facility delay or even prevent access to care. This has led to the development of integrated community case management (iCCM) initiatives, supported by the Pioneer project, that train village health teams on several health issues including diagnosis and treatment of the three most common childhood illnesses – diarrhoea, pneumonia and malaria.
Copyright Malaria Consortium/Tine Frank
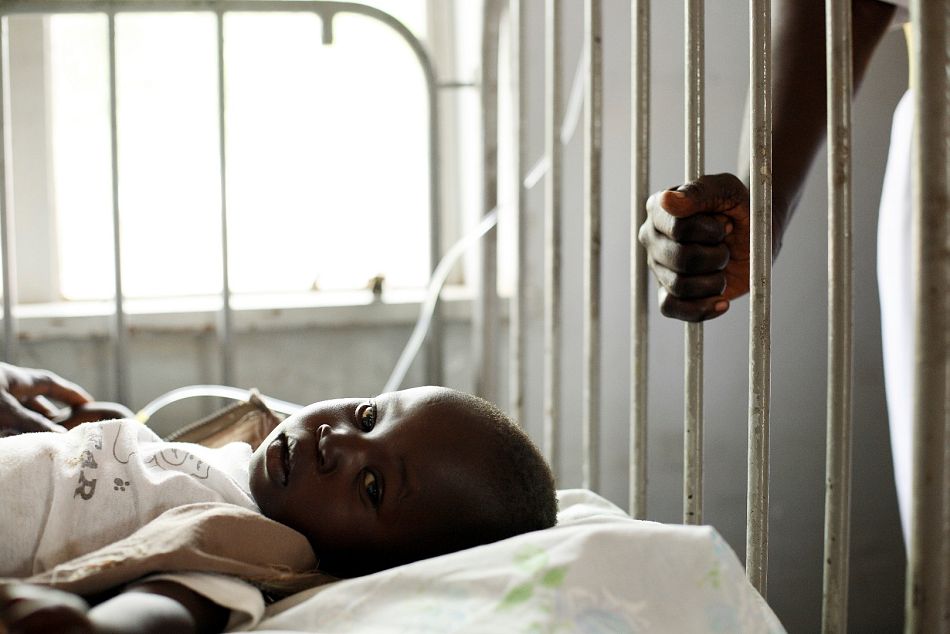
One key intervention for managing severe malaria is through rectal artesunate – a treatment that can slow down the disease’s progression in severe cases. This must be followed by comprehensive case management at a health facility and a full dose of antimalarial medicine.
Here, a father sits with his son, whose life was saved when the village health team provided rectal artesunate to buy enough time for him to get to the health centre.
Copyright Malaria Consortium
The Pioneer project also focused on encouraging the adoption of healthy practices. As part of the ‘Keep Good Health Enjoy Life’ campaign, Malaria Consortium encouraged the use of VHT services, daily use of mosquito nets and improved adherence to RDT results. Here, Mike Sebwufu stands in front of a sign at Lunya Primary School – one of the schools supported by Pioneer to implement behaviour change communication (BCC) activities. Efforts included a combination of radio spots, live talk shows, community dialogues, school programmes and the distribution of print material.
The Pioneer project has had a great impact on the lives and health of Ugandans. Not only in terms of net distribution and case management, but also in increasing demand for services and monitoring the effects of various interventions. The results and lessons learnt will help inform future malaria initiatives in Uganda. Find out more by reading our end-of-project report.
10
1
Country: Uganda
Keywords: Community delivery | Surveillance | Public health communications | Health system strengthening | Facility health services | Maternal, neonatal and child health | Preventive treatments | Diagnosis | Treatment | Vector control
Related content
26 February 2015Ugandan Pioneer Project unveils achievements and charts the way forward
Type: News article
26 September 2014Pioneer project 2009–2014: A holistic systems strengthening approach towards malaria control in midwestern Uganda
Type: Project report
28 June 2013Pioneer project and malaria in mid-Western Uganda
Type: News article