Ethiopia
In Ethiopia, around 52 percent of the population lives in malaria risk areas; pneumonia remains the leading infectious cause of death among children under five; and the country has one of the highest neglected tropical disease burdens in Africa. The Southern Nations Nationalities and Peoples’ Region (SNNPR) has one of the highest malaria burdens in the country, accounting for 18 percent of total malaria cases reported nationally in 2019/2020. We work closely with the government to strengthen the health system, reduce the malaria burden and tackle poor child health indicators including pneumonia.
Strengthening community-based malaria prevention and surveillance interventions
We will contribute to the sustained reduction of malaria in Wolaiyita zone of the Southern Nations, Nationalities, and Peoples' Region (SNNPR) in Ethiopia, by strengthening the management and technical capacity of the primary health care unit to maintain high coverage and the use of high impact anti-malaria interventions.
BREATHE - Breath recognition aid
to health experts
We undertook a study to develop an improved reference standard for counting respiratory rate through annotation software to help validate new automated pneumonia diagnostic aids for children under five.
Transform - Primary healthcare
We supported strengthening primary healthcare in Ethiopia to reduce preventable maternal and child deaths by supporting the implementation of the Government’s Health Sector Transformation Plan. The projecy aimed to improve the management and performance of Ethiopia’s health system, increase the sustainability and quality of service delivery across primary healthcare, improve households’ and communities’ health practices and health seeking behaviours and share learning to strengthen policies and practices.
ARIDA field trial acceptability study
We undertook trials of acute respiratory infection diagnostic aids (ARIDA) to determine if frontline health care workers in resource limited community settings and health facilities using respiratory rate counting aids are able to correctly assess and classify children under five with cough and/or difficulty breathing and explore the acceptability of these devices in this context.
Happy Feet: Accelerating the control of Podoconiosis in Ethiopia
The outcome of the project is to contribute to the reduction of the rate of new Podoconiosis cases through universal access to appropriate preventive and management health services, to less than one percent in districts where the project is active, by 2025.
Strengthening the pneumonia response in Ethiopia
In discussion with the Maternal, Child Health and Nutrition directorate of the Federal Ministry of Health, we are developing an action plan for the integrated management of newborn and childhood illnesses, focusing on pneumonia and diarrhoea, to support the existing newborn and child survival strategy and child health roadmap.
Determining the malaria burden and long-term complications following SARS-CoV-2 infection
This study is taking place in Ethiopia and Uganda. It uses both qualitative and quantitative approaches and a case-control study design to explore the relationship between past SARS-CoV-2 infection and malaria risk.
Malaria Consortium in Ethiopia
Malaria Consortium has been implementing projects in Ethiopia since 2004 from our offices in Addis Ababa and Hawassa, with a focus on the Oromia region and Southern Nations, Nationalities and Peoples’ region (SNNPR). We support the Ethiopian government in its efforts to tackle three major public health issues: malaria, neglected tropical diseases (NTDs) and poor child health indicators such as pneumonia and febrile illness.
Alongside our programmes, we have facilitated forums to coordinate stakeholders’ efforts and streamline the technical assistance provided to national and regional programmes through mechanisms including the Coalition Against Malaria in Ethiopia and the Malaria Control Support Team’s Technical Advisory Committee as well as undertaking pioneering research projects with the support of the Ethiopian Public Health Institute and others.
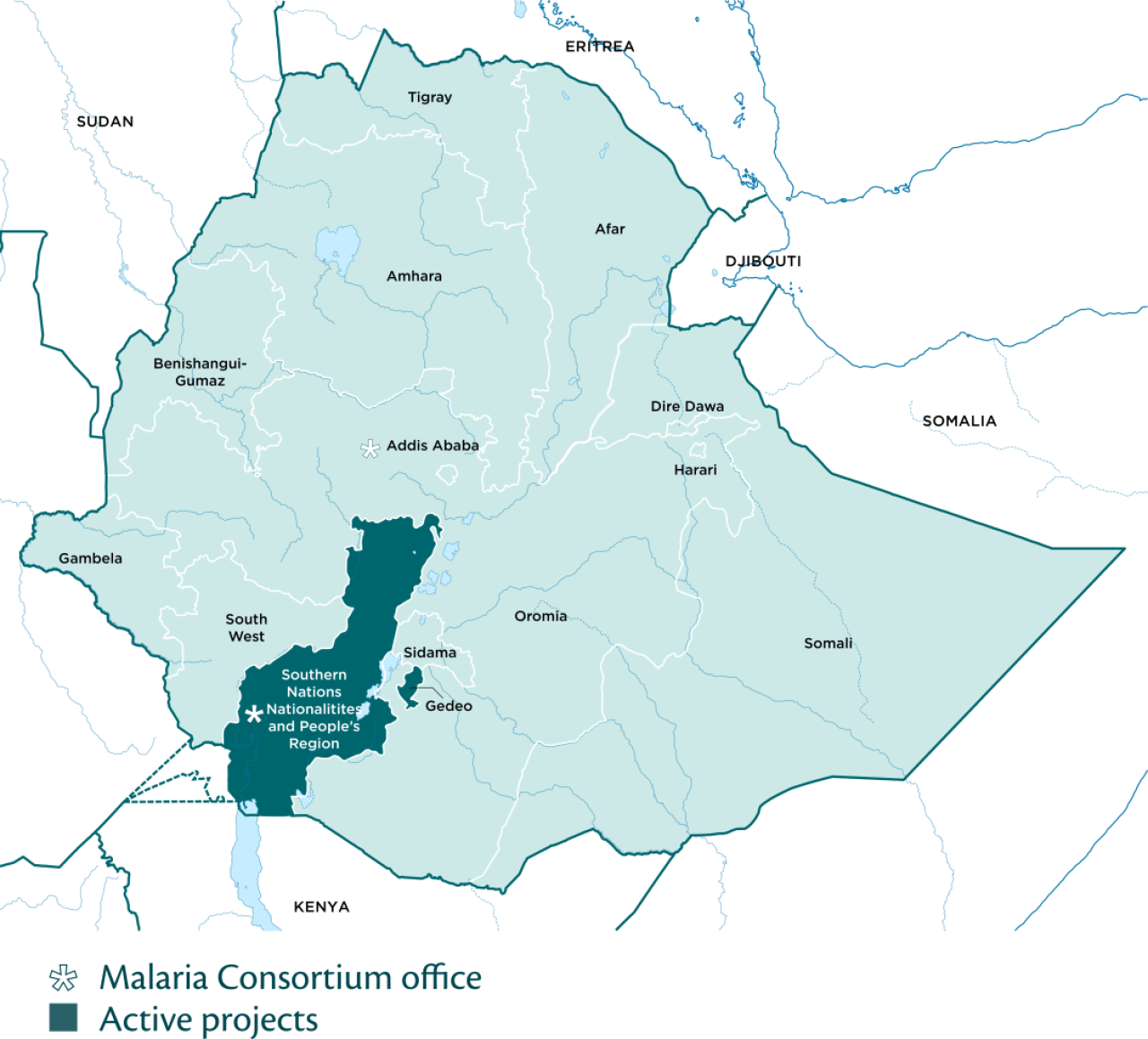
Areas of focus
Strengthening existing health systems is key to sustainably reducing malaria morbidity and mortality in Ethiopia. We offer technical expertise in malaria surveillance to assist decision-makers in gathering data to evaluate programmes and target scarce resources effectively. We are developing and setting up surveillance dashboards at district health offices and health facilities, with a view to enhancing the health system’s capacity to identify and respond to malaria outbreaks. We also plan to support the Federal Ministry of Health’s (FMoH) rollout of a new electronic community health information system to stimulate the use of data for decision-making. To further support health system responsiveness, together with the Ethiopian Public Health Institute, we were the first to monitor changes in malaria epidemiology in different endemicity settings in Ethiopia as part of the Beyond Garki project and have helped reduce malaria morbidity in the SNNPR by improving malaria diagnosis and case management at health facilities.
We promote social and behaviour change (SBC) interventions to ensure that the communities we work with are informed and engaged — supporting the practice of preventive health behaviours and community-led solutions. Through targeted, multi-level SBC approaches, we inform households of the importance of indoor residual spraying (IRS) and encourage them to use long lasting insecticidal nets (LLINs) correctly and consistently, seek healthcare early on and adhere to treatments. We have disseminated key public health messages through radio broadcasts, billboards and posters, mobile vans and community dialogues and, recognising schools as an effective entry point for SBC activities, developed School Club Guidelines for the SNNPR which have fed into the Federal Ministry of Health’s rollout of anti-malaria school activities in other parts of the country.
We support the government’s strategic objective of integrating interventions for neglected tropical diseases (NTDs) into the primary healthcare system. This is part of the country’s NTD Master Plan (2016–2020) and is in line the World Health Organization’s (WHO) NTD road map (2021–2030). Our operational research project in Ethiopia explores the feasibility, acceptability and cost-effectiveness of integrating interventions for lymphatic filariasis, schistosomiasis, trachoma and podoconiosis into the healthcare system. The latter is a non-communicable disease that affects over 1.5 million people in Ethiopia, but is little understood.
We support the implementation of the Ethiopian government’s Health Sector Transformation Plan to reduce preventable maternal and child deaths. Through the USAID-funded Transform: Primary Health Care (2017–2019), we developed the capacity of antenatal care providers to diagnose and treat malaria, as well as to record case management data in the regions of Amhara, Tigray, Oromia and SNNPR and worked to improve treatment of unclassified fever in under-fives by assessing health extension workers’ treatment of cases of unclassified fever and their follow-up recommendations. We have also pioneered digital health solutions to tackle pneumonia, introducing two automated respiratory rate counting aids and investigating the use of artificial intelligence to improve the ease of diagnosing pneumonia in children under five.
Related content
World Malaria Day 2024
 Page:
Page:About us
 Blog:
Blog:Published 7 March 2024
International Women's Day 2024: Seven ways to make health programmes gender intentional
 Page:
Page:International Women's Day 2024: Seven ways to make health programmes gender intentional
 Page:
Page:Our third year as an Independent Research Organisation: Using research to respond to health inequities and emerging threats
 Blog:
Blog:Published 20 February 2024
Our third year as an Independent Research Organisation: Using research to respond to health inequities and emerging threats
 News:
News:Published 13 February 2024
Scaling up key interventions could halve pneumonia-related childhood mortality
 Page:
Page:International Day of Women and Girls in Science 2024
 Blog:
Blog:Published 29 January 2024
Psychosocial and economic rehabilitation training essential to improve wellbeing for patients with podoconiosis
 Resource: Learning brief
Resource: Learning briefPublished 29 January 2024
Happy Feet: Initiating and integrating low-cost podoconiosis and lymphoedema management services in primary healthcare
 Resource: Journal article
Resource: Journal articlePublished 12 January 2024
Predicting the potential impact of scaling up four pneumonia interventions on under-five pneumonia mortality
 Resource: Annual review
Resource: Annual reviewPublished 2 January 2024
Trustee's report and financial statements for the year to 31 March 2023
 Page:
Page:Top reads of 2023
 Blog:
Blog:Published 15 December 2023
Top reads of 2023 Page:
Capacity statement: Ethiopia
 Blog:
Blog:Published 9 November 2023
Artificial intelligence among innovations supporting improved pneumonia diagnosis
 Resource: Advocacy brief
Resource: Advocacy briefPublished 31 October 2023
From steps to solutions: Advancing podoconiosis prevention and control in Ethiopia
 Resource: Annual review
Resource: Annual reviewPublished 18 October 2023
20 years of impact: Saving lives, transforming communities
 Page:
Page:20 years of impact: Saving lives, transforming communities
 Resource: Technical brief
Resource: Technical briefPublished 21 September 2023
Paving the way for universal health coverage
 Resource: Capacity statement
Resource: Capacity statementPublished 20 September 2023
Integrated community case management
 News:
News:Published 18 September 2023
African-led vector control solutions in the context of emerging threats
 Resource: Journal article
Resource: Journal articlePublished 21 July 2023
Usability of pulse oximeters used by community health and primary care workers as screening tools for severe illness in children under five in low resource settings
 News:
News:Published 18 July 2023
Thousands more children will survive by increasing access to pulse oximetry
 Resource: Capacity statement
Resource: Capacity statementPublished 14 July 2023
Malaria Consortium Ethiopia Page:
Prioritising the pneumonia and diarrhoea agenda in Ethiopia: Strengthening strategies for child survival Project:
Published 1 July 2023
Reducing malaria burden among seasonal mobile workers through innovative approaches in the Amhara Region
 News:
News:Published 13 June 2023
Ethiopia marks another milestone in its pneumonia and diarrhoea reduction plans