Helping Reduce Child Pneumonia Deaths in Cambodian Rural Communities
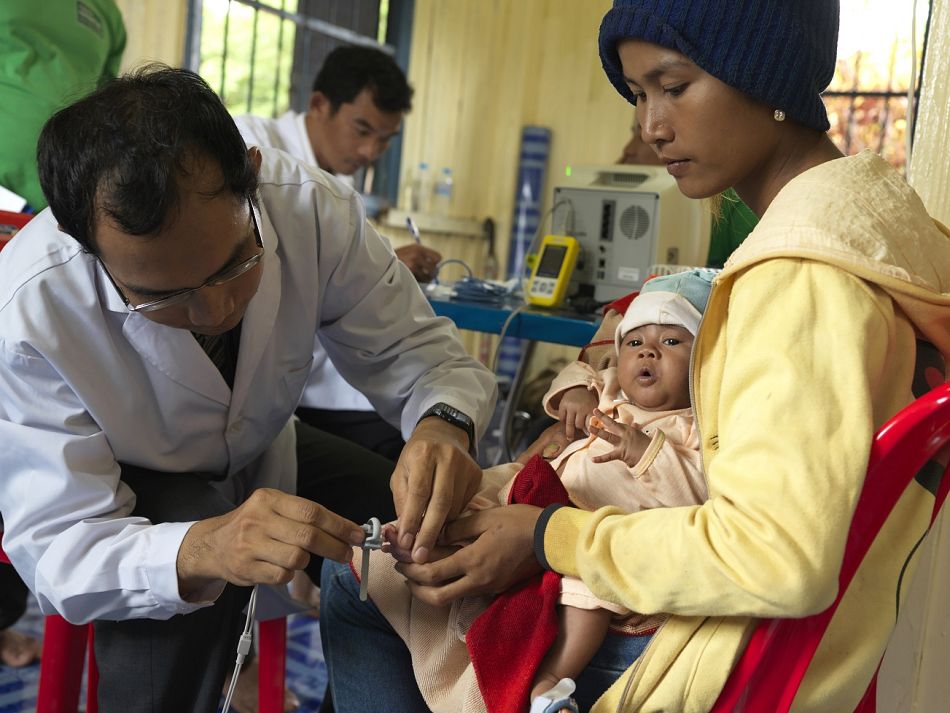
28 September 2015Rochom Wart is one of 65 village malaria workers (VMWs) in Cambodia, who has been trained to also detect the signs and symptoms of pneumonia in children under five years using special new diagnostic tools.
The new devices - pulse oximeters, which measure the levels of oxygen in the blood, as low levels are a symptom of severe pneumonia; and respiratory rate timers which help determine a child’s breath rate, as high breath rate is an indicator of pneumonia - are being tested for use by health workers at community and first level health facility levels across four low-income countries as part of Malaria Consortium’s Pneumonia Diagnostics Project.
“I think this study is important,” said Rochom Wart, a community health worker in Ratanakiri province, Cambodia. “With these devices, now we can see the results on the screen so we can quickly know if the child is sick or not. I am happy to participate in this study because before I did not know how to use the devices in order to know if it is severe pneumonia or not.”
Pneumonia is the number one infectious killer of children under five years old in Southeast Asia and sub-Saharan Africa. The mortality rate for children under five in Cambodia is amongst the highest in the region, with pneumonia accounting for between 16-30 percent of child deaths. Pneumonia deaths can be attributed to late care-seeking and inappropriate treatment due to misdiagnosis of symptoms.
The Pneumonia Diagnostics Project, funded by the Bill & Melinda Gates Foundation, will identify the most accurate, acceptable and user-friendly devices for use by frontline health workers. The four countries forming part of the study are Cambodia, South Sudan, Uganda and Ethiopia.
The first phase of the project involved a device selection stage where devices for diagnosing pneumonia in low-resource settings were systematically reviewed. After the most promising and appropriate respiratory rate timers and pulse oximeters for field testing had been identified, the next stage entailed exploring the accuracy of each device used by community and first level health facility workers against three reference standards.
Like Rochom Wart, a large number of health workers at community and first level health facilities in Ratanakiri travel daily from remote parts of the province to take part in the project.
“The training is very good and useful because I get more experience and gain more knowledge on pneumonia as a disease,” said Sol Leang, a VMW in Oyadav District, “Taking part in this study, I have learned about signs and symptoms of pneumonia and how to use modern devices to diagnose severe pneumonia.”
An especially motivating factor for many of those participating in the research study is the hope that they could eventually use the improved and easy-to-use technologies on children in their communities to help diagnose pneumonia as part of their day-to-day work.
“We can help the community with these devices. In case of severe pneumonia, we can refer quickly to hospital,”said Kay Raseu, a VMW from Ochum District. ”With these devices it is easy to assess the child, since I can see the results quickly.”
The next and final stage of the Pneumonia Diagnostics Project is the field evaluation, which will be conducted from September to November 2015. The field evaluation will assess the feasibility of introducing the devices into routine health worker practice at community and first level health facility level and explore the acceptability of the devices by both the health workers and the children’s parents or caregivers.
Monica Posada is the Behaviour Change Communication Technical Specialist at Malaria Consortium, Cambodia. She is in charge of providing technical support for projects that combat targeted diseases and promote child and maternal health trough sustainable and innovative public health communications.
Country: Cambodia
Keywords: Diagnosis
Latest news
- International summit calls for AMR accountability in public health interventions21st March 2024
- Global SMC community celebrates new milestone at SMC Alliance Annual Meeting in Nigeria6th March 2024
- Scaling up key interventions could halve pneumonia-related childhood mortality13th February 2024
- Malaria Consortium and eGov Foundation join Mozambique’s national malaria programme to digitalise seasonal malaria chemoprevention campaigns8th February 2024
- World’s first malaria vaccine rollout launched in Cameroon22nd January 2024
- Digital solutions driving equitable access to health6th December 2023