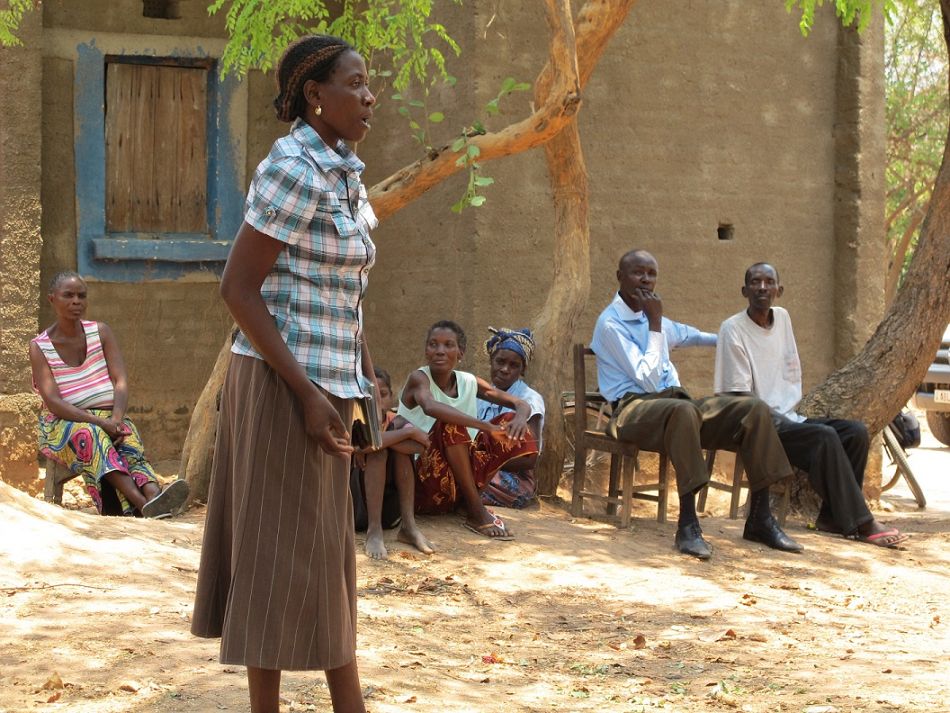Community dialogues in Zambia - in pictures
2 September 2014
The success of health interventions hinges on the involvement of affected communities. One method of encouraging engagement is through community dialogues, which gather villagers to discuss and find local solutions to health challenges.
Malaria Consortium has supported integrated community case management (iCCM) interventions to address the three biggest killers of children under five in Zambia: pneumonia, diarrhoea and malaria. Activities have been supplemented with community dialogues which are led by trained community health workers (CHWs), in order to raise awareness of the new health services available, and improve timely care-seeking in case of child sickness.
Check out the photos below to hear about community dialogues from members of two communities in Mwense district, Zambia.
Learn more about community dialogues in Zambia, Mozambique and Uganda by reading the learning brief here.
The community dialogues were held in Mwense district, Zambia. Malaria Consortium trained CHWs in the region to identify and treat the biggest childhood illnesses, including malaria, pneumonia and diarrhoea. In addition to acting as a first point of contact, they were also in charge of leading community dialogues, which provided a platform for all villagers to discuss health issues.
“This dialogue was just wonderful. This is what should be happening all the time instead of discussing politics only in community meetings! We learned a lot of new things, and corrected our misconceptions about malaria and especially the mosquito – now I know that only the mosquito causes malaria and nothing else and that early treatment is important and not to use traditional medicines first.” - Women from Mukomansala village in Zambia
“What I like about the community dialogue is that it is open to everybody, every community member, and it brings out issues, such as traditional practices, to discuss them openly. I noticed that people are eager to learn, to know about the diseases, and they are interested to know what actions they can take. They ask a lot of questions! The flash cards are very helpful because they show the route to keep the child healthy and the different steps on this route. Because they can visualise with pictures, it is easier for them to understand and to remember.” - Kaulu, Headwoman in Mukomansala village
Trained facilitators ask villagers to share their own stories of what happened the last time their child fell sick. What did they do? When and where did they look for advice or care? And what was the outcome? They can share their story by placing images on the poster; then the group discusses the best route to ensure the child receives appropriate care. This allows for tackling local practices such as delay in care-seeking, the use of traditional herbs, among others. Visual materials and flashcards help caregivers identify symptoms and follow the correct procedures when their children get sick.
“About a month ago, my baby fell sick. The next day, I rushed to the CHW. It was the first time I consulted him actually. We call him Mr Joe. When I arrived, he greeted me, offered me a seat and asked me what the problem was with my child. So I explained to him that the boy was feverish and also coughing. So, he pulled out a thing that beeps and showed some light and numbers and made some sound like ‘tata’, and I saw him start counting. So I was surprised and I asked: ‘are you going to know if my child is sick by doing this?’ And he said yes – he explained he was counting to check if the child was breathing faster than normal.” – Barbra, from Chabala village
“Usually, people tend to keep sick children at home and to use some traditional herbs to heal them. They tend to use traditional medicine because this is all they know; but they don’t dare to tell us at the health centre what they actually do; they keep quiet; whereas during the community dialogue, they talk freely and the traditional practices come out. This community dialogue is the right platform for unveiling these practices and discussing openly about the risks and benefits for the child’s wellbeing.” – Mwila is an Environmental Health Officer and has trained facilitators for community dialogues. He uses his motorbike to travel to villages in order to provide outreach services such as immunisation.
Community dialogues have increased awareness among community members on the importance of early care-seeking in case of child sickness; early care-seeking can save lives. “I remember a case referred last month by one of our CHWs. The parents were out in the bush with the child to do some farming. Then the child fell sick, and the parents realised it was quite serious so they came back to the village. But they did not call for help; actually they just kept the sick child at home. Until a neighbour realised this child was very sick, and alerted the CHW. The CHW immediately went to see this child; the child had severe headache, fever and fast breathing. The CHW decided to refer the child to the health centre. The parents made it up to the hospital, and the child recovered within five days."
“The communities around are very receptive; they welcomed this new health centre; we are also working very well with the CHWs. When they were just freshly trained in ICCM, they were not always very confident to diagnose and treat, especially with pneumonia. At the beginning, we could see from their reports, that they prescribing a lot of antibiotics; so we investigated and we discovered that some of them would give antibiotics for simple cough and not only for pneumonia; so I have supervised them and now I can see that they are diagnosing properly. They deliver antibiotics only to children with fast breathing rate, with a clear sign of pneumonia, but not to children with simple cough.” – Elizabeth is sister in charge at Musonda Health Centre.
9
1
Country: Zambia
Keywords: Public health communications | Community delivery